Health, safety, staffing concerns stack up for Glenwood Springs nursing home
New management says it's working to address mostly pre-existing problems
tflowers@postindependent.com
Marvin King says his father Tommy King fell on the way to the bathroom one day at Glenwood Springs Health Care.
Both men say Tommy laid on the floor for about 30 minutes before he was finally able to pull himself back onto his bed.
King said he noticed red flags just hours before his father was admitted to the local nursing home in February.
On the morning of his father’s admittance, staff was still scrambling to verify Medicare approval and payment, King said. When staff finally checked the 68-year-old into the facility, he was almost a full business day late, missing dinner, and his daily medications.
“It has not always been a bad facility. Madison has a pretty good reputation. It’s the people you put on the ground in these facilities that makes or breaks you.”—Bob Spuhler, ombudsman
“He’s 100 percent disabled,” King said of his father. “When you have a critical care patient, they’re supposed to get what they need when they need it.”
King’s father sustained a long list of injuries while serving in the Vietnam War. He now requires a pain pill every four hours and a host of other medications that treat type II diabetes, chronic obstructive pulmonary disease, bone degeneration disease, neuropathy, and neck, rib, and spine damage.
“He went like 11 hours without medication the first night he was there,” King said.
When his father asked for the low carb, low sugar diet he uses to help manage his diabetes, staff allegedly said he needed to see a doctor first.
“He had me come pick him up because he was scared he was going to die and he called me crying and begging,” King said of his father.
King only lasted there three days.
STATE INFRACTIONS
Marvin King isn’t the only critic. Residents and former employees expressed similar concerns.
The facility has routinely received low ratings from regulators and it has a list of health care “deficiencies” from the state health department, which conducts unannounced annual inspections.
“It’s those surprise visits that are often the catalyst for the biggest change in facilities because they’re not prepared for them to show up,” said Dr. Sheri Gibson, steering committee chair for Colorado Coalition for Elder Rights & Abuse Prevention.
“Unless you have somebody who is there 24/7 monitoring every single thing, yes things can fall through the cracks,” she said.
 The facility’s administrator, Chavien Paget, said he is aware “the nursing home’s history isn’t super favorable” and that he and the director of nursing are working to clean up the facility’s reputation.
The facility’s administrator, Chavien Paget, said he is aware “the nursing home’s history isn’t super favorable” and that he and the director of nursing are working to clean up the facility’s reputation.
Paget and Jenny Sickles, the director of nursing, said the facility has received fewer “tags” or deficiencies since they were hired in August and November 2017, respectively. Sickles said the facility had about 20 “tags” under previous management in 2016, but under her current supervision, that number has fallen to 14.
“It’s a long road and we have a long history of not so great things to combat but we’re trying everyday,” she said.
Glenwood Springs Health Care (formerly known as Grace Health Care under previous ownership) is now owned by Madison Creek Partners. It was ranked the ninth most cited nursing home in Colorado until this month, when its number of deficiencies dropped from 58 to 50, according to U.S. Centers for Medicare & Medicaid Services.
Those 50 “healthcare deficiencies” have been recorded since 2015, according to ProPublica, a news organization that aggregates data from Centers for Medicare & Medicaid Services.
Paget and Sickles said deficiencies remain on a nursing home’s record even after they’re addressed to educate the public about a nursing home’s history. Paget and Sickles said all 50 deficiencies have been cleared by the state.
According to the most-recent data compiled by Centers for Medicare & Medicaid Services, it’s now ranked among the top 20 most cited nursing homes in the state. There are 229 nursing homes in Colorado.
Colorado’s Department of Public Health and Environment keeps state health inspection reports, and the Department of Health and Human Services for Medicare & Medicaid Services compiles its own version of that information, which one can cross-reference.
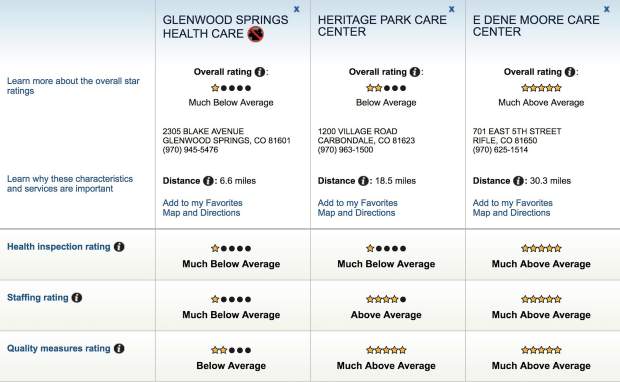
In comparison to the 20 other nursing homes within 100 miles, it’s ranked the lowest across four categories, which includes health inspections, staffing, quality measures, and overall care. Reports are available to the public.
“I’ve told people, if you do not like your family member, that would be the place to send them,” said Tushina Sanderson, a former certified nursing assistant, who left the facility in February.
“As far as safety, the aides don’t use the gait belt,” a device that helps secure residents with balance issues and assists caregivers with proper transfers, she said.
Sometimes aides transfer residents on their own when the maneuver requires two people, and that can cause tears to older skin, which becomes less elastic from time and medication use, she said.
Paget, the building’s administrator, said he is aware of “trends” like skin tears and he’s working to improve management over all. He says, under his supervision, he has incorporated a new system, in which each of the building’s manager’s conducts “angel rounds,” by asking residents if they have and concerns, and if grievances are addressed when filed.
But he maintained those issues aren’t rampant under his current supervision. “All the negativity is from before us,” he said.
Sanderson said she resigned this year, after nine months, because she felt she couldn’t adequately do her job.
“I left because of upper management not taking care of what needed to be taken care of,” she said.
The facility has paid more than $130,000 in fines in the past three years. That’s the 11th highest penalty among the 228 other nursing homes with infractions in the state.
To put that into perspective, Alpine Living Center in Thornton has 93 deficiencies, the highest in the state, and Yuma Life Center in Yuma paid the heftiest fine of more than $546,000.
“It’s not just this nursing home, but this one was beyond horrendous in my eyes,” King said of Glenwood Springs Health Care.
Conversely, eight Colorado nursing homes have maintained a clean record since 2015, with no deficiencies or fines, including two others on the Western Slope in Grand Junction. One nursing home in the state, Belmont Lodge Health Care Center in Pueblo, is flagged for having a history of serious quality issues.
Nursing homes across the country face allegations similar to King’s and many receive citations for healthcare infractions when investigators find wrongdoing. Disciplinary action can include hefty fines, staff firings, integration of new policies, and additional unannounced state health inspections.
CHRONIC UNDERSTAFFING
Understaffing is one of the main contributors to poor and inadequate care, said Lori Smetanka, the executive director of the National Consumer Voice for Quality Long-Term Care, an organization that formed in 1975 amid growing public concern about subpar care in nursing homes.
According to the Colorado Secretary of State, nursing homes in Colorado must employ at minimum one full-time registered nurse, a full-time director of nursing, and a licensed nurse on each unit.
If a facility is staffed sufficiently, the site says, it will be able to provide at least two hours of care to each patient per day.
But it would be impossible for three staff members to provide that level of care at a facility like Glenwood Springs Health Care, which houses 56 residents at capacity. Nursing homes in rural areas can legally waive that number if they have trouble finding or maintaining the three staff members per shift, according to the state.
Last year, as reported Thursday, the Glenwood facility got burned when officials investigated an unlicensed nurse who had worked at the facility. She had been hired in an administrative capacity and promoted to “nurse” to help alleviate problems of understaffing, even though she was unlicensed and never held a nursing degree.
But Sickles and Paget maintain they are not currently understaffed. They said eight employees work during the day, two nurses work at night before 9 p.m. and after that, one nurse is available. They maintained one nurse is sufficient after 9 p.m. But Sanderson, residents, and inspection reports say understaffing is an issue, especially at night.
Sanderson, the former employee, said many residents don’t need the level of care the nursing home provides and that if they were cared for elsewhere, that would alleviate the understaffing issue.
“I think it’s, however we can fill this bed to make that money, then that’s what we’re going to do,” she said.
Sickles, the director of nursing rebutted, saying Garfield County officials conduct an assessment and decide if residents qualify for the level of care at the facility.
Sanderson said she wasn’t properly briefed on “charting” or documenting residents’ weights and vital signs, and to save time, staff would “cut corners” and omit documenting residents’ daily fluid and food intake.
“I would get in trouble for spending too much time in a resident’s room [when] they needed someone to talk to,” she said. “They teach you how to cut corners when [the] state’s not there.”
Part of her responsibility as a certified nurse’s assistant was to bathe residents in the “bath house,” and she says she would take her time washing residents, often blow-drying and styling their hair. But that caused contention too.
“I’m not just going to go in there and spray them down and then wheel them out. Part of our job description was to take care of them,” she said.
According to the most recent inspection, conducted in January of this year, one employee was fired in January for speaking to residents in an “inappropriate manner.”
The reports say a resident was given anti-depressant medication for two and a half months, even though he or she never signed a form consenting to it. And, residents complain the facility runs out of medications because they’re not reordered in time.
In that same report, a 70-year-old “severely cognitively impaired” resident’s treatment plan said she was supposed to wear special knee high stockings for an unspecified leg condition but the resident told inspectors the stockings were rarely applied. Inspectors, who said the resident’s legs were “extremely” affected by her medical condition, say in reports, on three separate occasions, the resident was seen not wearing the stockings.
In 2016, before Paget and Sickles arrived, an annual inspection showed understaffing had resulted in delayed call light response, late assistance to the toilet, and subpar bathing. Residents quoted in the reports said they felt helpless and embarrassed as a result.
COMMON ISSUES IN RURAL AREAS
Dr. Gibson, of Colorado Elder Rights Coalition, maintains that rural areas especially struggle with high turnover. She said losing a certified nurse assistant incurs an astronomical expense and could cost a facility more than $10,000 to train new hires and compensate others to cover empty shifts.
“If you have four or five people quit, that’s a huge loss to the organization,” which could in turn affect patient care, she said.
Sanderson said another factor many don’t consider is, “The heart that it takes to take care of these people, because they’re not easy,” she said.
“They swing at you, they bite you, they pull your hair,” she added. On one occasion, a “frustrated” resident with dementia pulled Sanderson’s hair and she decided to cut it, as a result.
“The issue for a lot of these facilities is that they are under staffed, poorly funded, and they are working under the context of providing care to the frailest individuals in our community, our loved ones,” Dr. Gibson said.
With the mandated staff-to-resident ratio, “They have real challenges around staff retention and meeting the demands of their residents,” she added.
According to historical references in state documents, in 2007, when the facility was known as Grace Health Care and was under different ownership, it revised its policy on staffing and vowed to provide adequate nursing, to meet the needs of its resident population. But current residents say they’re still not receiving the appropriate level of care.
Sanderson echoed their concerns, saying complaints are rarely addressed and she’s unsure if residents know they can file complaints with the state health department. Even if they do, she said, many don’t have the capacity to successfully complete the forms on their own.
Even when the state is involved, residents say their needs aren’t always met. A female resident, who spoke on condition of anonymity, pointed to the most recent grievance dated May 23, which resulted in no action taken, according to the state’s website.
A representative from Colorado Department of Public Health and Environment, which compiles the reports, said she wouldn’t disclose any information regarding the nature of the allegations or what the investigation found, since no citations were issued in regard to incident.
“With the complaint, we look for a point in time,” said Lorraine Dixon-Jones, a former policy advisor with the state health department.
“So, maybe trash was piled high on Thursday, we go Monday, and there’s no trash,” she said. “We have to have enough evidence that it happened,” she said.
Her comment was in response to a former employee’s concerns about trash cans allegedly overflowing with diapers and human excrement.
Paget, the facility’s administrator, said he is held accountable by the ombudsman monthly and that he has worked to resolve grievances.
“I think we have been doing a better job than has been done historically in the building,” he said, adding that he encourages residents to share their concerns.
Previous infractions mirror current allegations, and falls similar to King’s are fairly common.
On one occasion, in October 2016, an 89-year-old man sustained a head laceration when he rolled off his bed, a witness said. Reports say his head was bleeding profusely before he was rushed to the emergency room.
Inspectors say staff developed a fall prevention plan for him but it hadn’t been updated, even though he had fallen five times since its implementation.
There were no follow-up investigations or neurological checks documented in the resident’s chart and inspectors say staff listed he was at “low risk for falling,” even when he had fallen that same day. One LPN told inspectors he might have fallen twice in six days, according to the reports.
During interviews conducted by the state, staff could not outline specifics about the resident’s injuries, which inspectors attribute to the lack of documentation in relation to the incident.
Two months before, a female resident fractured her ankle after falling on the way to the bathroom and was found lying on the floor yelling for help, according to the reports.
Documents say staff suggested she use her call light for help but she told them it was unplugged that day.
Current residents say those who are cognitively impaired are most often left dirty, and when staff is notified, they either brush off the information or say they’ve already cleaned the tenant.
“They have to sit in wet pads and clothes,” one resident said of a roommate, who needs around-the-clock care.
“Those kinds of things are commonplace in homes that neglect their folks, and unfortunately, are commonplace here,” the resident said.
In February 2017, a resident in her 40s was found to have an “open superficial area” to her labia, according to state health inspection reports.
The occurrence resulted from the lack of proper perineal care, from nurses not repositioning the resident, who is paralyzed from the waist down.
A staff member assigned to the resident admitted she hadn’t provided the appropriate care and said she was “unaware she was supposed to do this,” that the woman usually requested the care when she needed it.
The nurse was fired and reported to the Board of Nursing, and two days later an in-service training was scheduled to discuss proper positioning, abuse and neglect, according to state inspection reports.
“I loved my job but had to quit,” said a former employee, who spoke on condition of anonymity. “I couldn’t bear seeing what they were doing.”
A resident who’s also a former nurse says medications aren’t stored properly nor are they dispensed sanitarily or in a timely fashion.
Inspection reports support that claim in detail, stating residents are sometimes given psychotropic drugs when they haven’t shown symptoms of a mood disorder in weeks.
MANAGEMENT CHANGES
The facility’s ombudsman, Bob Spuhler, says he’s heard residents complain about delayed refills on medications.
“There are issues going on,” and there are “people looking into those issues,” he said without elaborating.
The “issues being looked into” are different from the allegations mentioned above, he said.
A previous administrator started making improvements by trying to rehabilitate the facility’s reputation, Spuhler said.
The facility, formerly called Grace Health Care, received fewer citations and a long list of to-dos dwindled under former administrator, Julianne Mobley.
But when Mobley announced the owners were selling the property in July 2016, the director of nursing and others in key positions left, Spuhler said.
The current owner, Madison Creek Partners, had to hire new staff, “and in that turmoil, things started falling into the cracks in my opinion,” Spuhler added.
“What happened in the turnover is they started losing all their leadership people. The new [computer] system got them back into the situation they were in before, in which things weren’t going well,” he said.
“It has not always been a bad facility. Madison has a pretty good reputation. It’s the people you put on the ground in these facilities that makes or breaks you,” he said.
RESOURCES AVAILABLE
Residents who disclosed the aforementioned allegations said they had never spoken publicly about their concerns. A group of residents who spoke under a gazebo outside the facility said they hoped doing so would inspire widespread change.
Dr. Gibson trains nursing home staff on compassion, fatigue, and burn out. She said those issues arise from rampant understaffing in both rural and urban areas.
When staff is burned out they start avoiding tasks and are frequently absent, she said.
“There’s a wide range of symptoms that show they’re burned out,” and “administrators need to notice the symptoms of their staff and offer ways of self care,” she said.
King, whose father allegedly fell at Glenwood Health Care said he never reported the incident because, “One, I felt like it was a waste of time,” and two, his wife was in the nursing profession and he and his father feared retaliation from her employers.
Dr. Gibson said residents who feel comfortable advocating for themselves, have the option to file grievances within and separate from the facility. Family members can step in and help with communicating concerns to the executive director to ensure they’re addressed, she said.
When residents fear retaliation and don’t have the support of a loved one, they can speak to the facility’s ombudsman, who works to ensure resident’s rights are protected, Dr. Gibson said.
Sanderson said when she took the job at Glenwood Springs Health Care, she heard the current manager was working to change its reputation but within the first week she noticed widespread health and safety issues.
King also said he was unaware of the facility’s reputation and he didn’t think to research the nursing home because he was referred there by another hospital.
There are many resources one can use when choosing a nursing home, as reported by the Post Independent last month.
U.S. Centers for Medicare & Medicaid Services, ProPublica, and state health inspection reports provide a wide variety of resources and gives readers a glimpse of a nursing home’s history and overall reputation.
When a VA hospital in Rifle couldn’t provide adequate care, King said he decided Glenwood Springs Health Care would be a better option for his father. But on the third day of his stay, when he left the facility, King’s father said he wanted to return home to his old doctors in Wisconsin.
“He decided to go back,” King said of his father. “He wasn’t going to die in Colorado. He was going to go home.”
But King said in Wisconsin, his father is still not receiving the care he needs.
Doctors at Twin Ports, a senior living facility in Superior, Wisconsin, are administering King’s medications on time, but staff keep rescheduling his appointments and he hasn’t had his pacemaker checked in a year, King said. They don’t have the budget, they’re understaffed, and they’re probably overworked, King added.
For King and his father, accessing health care has been an exhausting and redundant battle and he says his experience is representative of a much larger picture: Americans’ struggle to access the health care they need.
King said he takes 14 pills per day and has his own ailments, including degenerative bone disease and neuropathy, like his father. He was born with one kidney and has stage four renal failure because of his father’s exposure to agent orange while fighting in the Vietnam War. “And the government won’t do anything for me,” King said. “The health care in this country is a joke.”

Support Local Journalism

Support Local Journalism
Readers around Glenwood Springs and Garfield County make the Post Independent’s work possible. Your financial contribution supports our efforts to deliver quality, locally relevant journalism.
Now more than ever, your support is critical to help us keep our community informed about the evolving coronavirus pandemic and the impact it is having locally. Every contribution, however large or small, will make a difference.
Each donation will be used exclusively for the development and creation of increased news coverage.